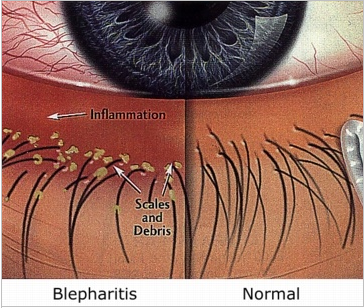
Blepharitis is a condition which causes chronic inflammation at the base of the eye lashes. The signs are often not easily seen, but examination with a microscope reveals crusting and scaling. This build up in turn can harbour low grade infections, and generally cause irritation to the eyes and lids. It is easily treated with routine eyelid hygiene, but this is a long term management strategy.
Previously it was common to recommend bathing the eyelids with diluted baby shampoo. Recent studies have suggested the shampoo can actually aggravate blepharitis. Instead we recommend wipes or gels and foams designed specifically for the eyelid. A number of the treatments include tea tree oil in the ingredients - this is very helpful in many cases.
If you are starting treatment we recommend daily lid hygiene for 10 days, then reduce to three times per week for maintenance. Remember blepharitis in most cases is chronic so you should be prepared to build lid hygiene into you everyday routine.
It is not uncommon for eyelids to become irritated when you first begin treatment - this should settle as the blepharitis comes under control. Here is an outline of the available treatments.
Lid wipes - these are convenient and come either in individual sachets, or a tub. Use one wipe each time, dedicate a fresh side to each eye lid.
Foam/gel cleaners - can be used in the shower. You are aiming to massage gently into the base of the eyelids, imagine shampooing the eyelashes. Rinse well or wipe off with a flannel.